Cases of type 2 diabetes are increasing dramatically worldwide. They are closely related to the obesity epidemic. In fact, type 2 diabetes is said to be in some ways a lifestyle disease.
537 M
This pandemic is increasing exponentially: in 2014, 537 million people were affected (Diabetes Atlas IDF 10TH Edition 2021). In 2050, an estimated 1.31 billion patients are estimated to suffer from type 2 diabetes1.
2 million
Diabetes and kidney disorders related to the disease were responsible for around 2 million deaths in 2019, according to WHO. 50% of people living with type 2 diabetes also have kidney disorders2.
95%
Type 2 diabetes accounts for 95% of global cases of diabetes.
The diagnosis rate of type 2 diabetes varies widely from country to country but is generally estimated to be between 50% and 70%. This means that up to half of all people with type 2 diabetes are unaware of their condition.
An estimated 240 million adults worldwide are living with undiagnosed diabetes. This represents almost half of the total estimated number of cases (Diabetes Atlas Greater Paris, 10th Edition, 2021).
A lifestyle disease
Non-insulin-dependent diabetes
Type 2 diabetes (or non-insulin-dependent diabetes) is a chronic excess of glucose concentration in the blood, or hyperglycemia. This condition is due to poor secretion of insulin (a hormone that regulates blood sugar) by the pancreas and to insufficient effects of insulin on target organ cells (liver, muscles, fatty tissues) – known as insulin resistance.
A silent disease
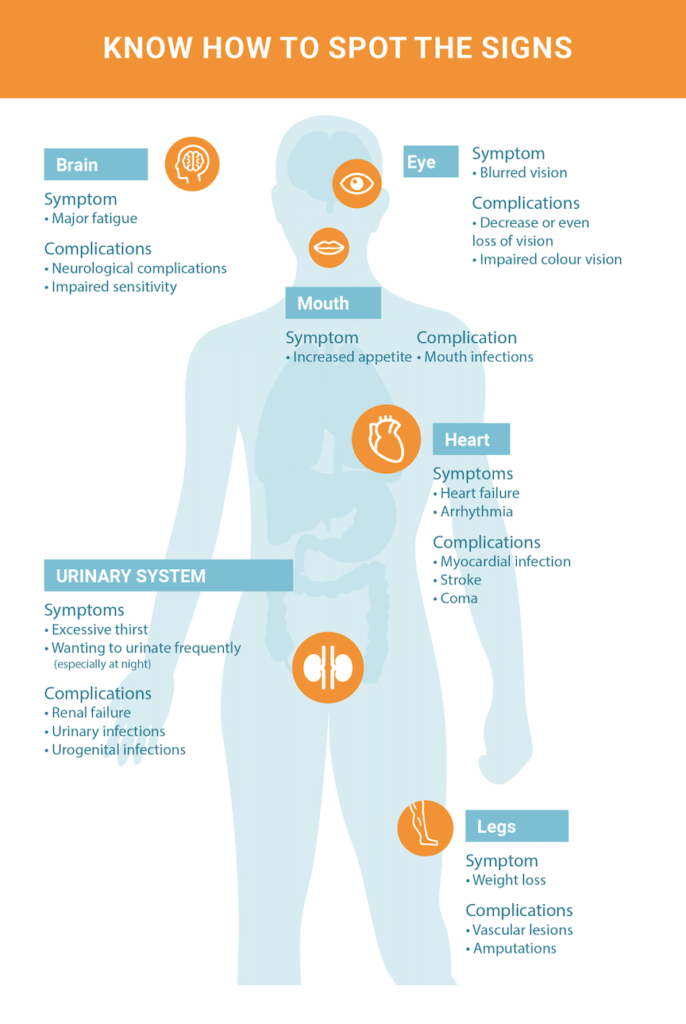
Most of the time, chronic hyperglycemia is asymptomatic. This is why according to estimates, 30 to 80% of diabetics are not diagnosed. Diabetes is diagnosed either through a routine blood test, or when complications appear, which makes them all the more serious.
Combat diabetes with changes in lifestyle
Measures to improve lifestyle quality may be sufficient to regulate type 2 diabetes. Losing weight if necessary, exercising, and adopting a healthy diet are part of standard treatment. This includes, for example, limiting intake of sugary, salty, or fatty foods; choosing fresh fruit and vegetables, eating more fish.

In case of failure to reach glycemic target, oral antidiabetics may be prescribed. There are several. Each one has different mechanisms of action and can be administered alone or in combination. Adopting a healthy lifestyle increases their effectiveness.
Living well with your diabetes
Books and information have been published to share “tips and tricks” to live better with type 2 diabetes. From healthy gourmet recipes to advice on the best sports for patients with diabetes, we now have an abundance of information at our fingertips. This is a great help for people who need to change their lifestyle. In addition, therapeutic patient education has been proven to improve the quality of life of diabetic patients.
REMEMBER

AND SERVIER?
We are committed to treating type 2 diabetes, and have launched several initiatives to help improve patient care and quality life.
The Group’s research is heavily involved in understanding the pathophysiology of type 2 diabetes and identifying new therapeutic targets in order to improve patient care and prevent complications.
For example, our MyHealthPartner website offers a wealth of information on chronic diseases such as type 2 diabetes. It aims to enable patients to better understand their condition and to support them on a daily basis at each stage of their journey.
Last but not least, since 2020, through our global awareness campaign #ACTNOWFORDIABETES, we continue to inform and raise awareness on the importance of early diagnosis of type 2 diabetes and treatment adherence.
